1. Acute Generalised Exanthematous Pustulosis (AGEP)
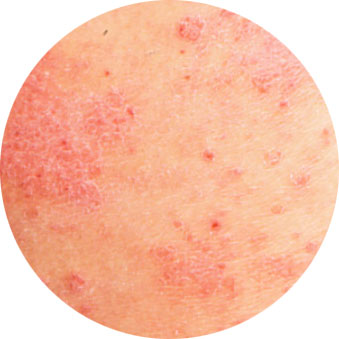
In AGEP, there are multiple non-infective pustules which may develop in the skin folds or all over the body. The rash usually happens less than 4 days after starting a drug, and is frequently accompanied by fever and an elevated white blood cell count. This reaction is self-limiting with a good prognosis in most cases after discontinuing the culprit drug. Common medications which cause this type of reaction include penicillin antibiotics.
2. Drug-induced Hypersensitivity Syndrome (DIHS)/ Drug Rash with eosinophilia and systemic symptoms (DRESS)
DIHS, also known as DRESS, is characterized by a conglomeration of symptoms and signs which include fever, extensive or generalised itchy red rashes and internal organ dysfunction. There may be enlargement of lymph nodes, elevated white blood cell count, raised blood eosinophils. Internal organs which can be affected include the liver, kidneys, thyroid gland, heart and lungs. Viral re-activation has been associated with DIHS. In most cases, DIHS occurs 2 to 6 weeks after initiation of the drug. The mainstay of treatment of DIHS is systemic corticosteroids. Cautious taper of systemic corticosteroids is often needed as abrupt cessation has been associated with flare of the condition. DIHS is associated with significant morbidity and mortality. Drugs which can cause DIHS include some of the anticonvulsant medications and sulphur antibiotics.
3. Generalised Exfoliative Dermatitis (GED)
There are many causes of GED. Hypersensitivity to drugs is one such cause. In GED, there is generalized inflammation of more than 90% of the skin surface, which may appear as widespread skin redness and scaling. Itch is usually present. Some patients may have associated swelling of lymph nodes, liver and spleen. Typically, GED occurs 1 to 6 weeks after initiation of the culprit drug. Complications such as inability to control one’s body temperature, blood fluid and electrolyte imbalance, infection and heart failure can occur. Prognosis is usually good after withdrawal of the offending drug. Oral corticosteroids may be necessary in severe cases. Drugs which can cause this kind of reaction include anti-TB medications.
4. Stevens-Johnson Syndrome (SJS) & Toxic Epidermal Necrolysis (TEN)
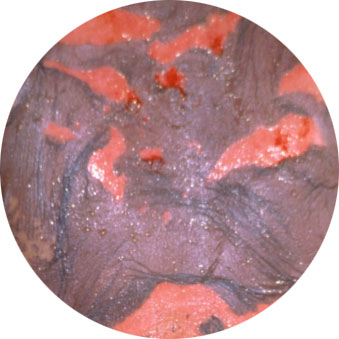
SJS and TEN are among the most severe drug eruptions. Characteristically, they affect the skin and mucous membranes. SJS and TEN are often preceded by a prodromal phase of fever, cough and malaise. This is followed by an acute red rash that progresses to widespread skin detachment, as cell death causes the superficial layer of skin (epidermis) to separate from the deeper layer (dermis). Red and sore eyes, as well as ulcers affecting the mucous membranes of the oral cavity, lips and genitalia are common features. SJS and TEN typically occur 7 to 21 days after initiation of the drug. They are associated with significant mortality and morbidity. Early diagnosis with prompt withdrawal of the culprit drug can lead to better outcomes. Patients should be hospitalized for close monitoring, supportive care and specific treatment. Drugs which can cause SJS/TEN include anticonvulsant medications, sulphur antibiotics or various other antibiotics and NSAIDs.