Fungal Infection (Ringworm, Tinea Capitis)
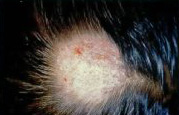
Ringworm infection of the scalp is caused by a fungal infection. Ringworm infection of the scalp is more common in children than in adults. Fungal infection of the scalp presents in a variety of ways, depending on its severity and source of infection. In mild cases, the fungal infection appears as itchy scaly patches on the scalp. The hair follicles and hair are infected. The infected hairs are irregularly broken and fall off leaving bald patches (Fig. 6). The underlying skin may be red and inflamed. In severe infection (often infected from infected pets), the scalp skin becomes very red, tender and boggy. Pus may exude from the inflamed skin and boils/abscesses (called kerion) may form. Infected hair falls off and crusting may be present.
Fungal infections of the scalp can be effectively treated with oral antifungal drugs and good hair care. The source of infection e.g. pets should be treated simultaneously to prevent recurrence. Early recognition and treatment of the fungal infection will prevent permanent scaring and balding. Consult your doctor immediately if you suspect you have fungal infection of the scalp.
Bacteria Infections Of The Hair Follicles (Folliculitis, Boils)

Bacterial infection of the hair follicles causes folliculitis, or inflammation of the hair follicles/pores (Fig. 7). Folliculitis presents as pimple-like eruptions on the scalp. The small, discrete red lumps are painful and tender and are often scattered on different areas of the scalp. Pustules may be seen. Some individuals are more susceptible to such infection than others. If the infection becomes too frequent, tests should be carried out to ascertain if there is any abnormality in their immune system.
Folliculitis can be effectively treated with appropriate oral antibiotics. Good hygiene, regular washing of the scalp and hair with mild antiseptic shampoo will help prevent recurrences. Occasionally long term oral antibiotics may be necessary to suppress infections.
Shingles (Herpes Zoster)
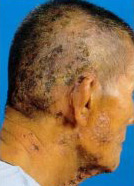
Shingles is caused by a viral infection. This virus also causes chickenpox. Patients with shingles always have past chickenpox infection. Shingles represent a reactivation of the chickenpox virus. It is often seen in individuals with lower immunity e.g. following a viral infection, cancer, etc. The skin eruptions appear in a linear pattern following the distribution of a branch of the nerve. There is often preceding pain and itch just before the appearance of skin eruptions. It presents as a very painful blistering rash followed over the next week by erosions and crusting over affected areas of the skin e.g. on the forehead and anterior scalp, or the neck and back of the scalp (Fig. 8). The condition is self-limiting and should clear after about two weeks. However, severe pain may persist for months after the skin lesions have cleared. The elderly are at a higher risk of developing post herpetic neuralgia. Patients with shingles should see their doctor and may require investigation for any underlying cause of lowered immunity.
Shingles can be effectively treated if appropriate antiviral drugs are taken very early (within 48 hours of appearance of symptoms). Oral antiviral drugs can reduce the duration and severity of shingles. Consult your doctor immediately if you suspect you have shingles. Fig. 8 Vesicles, erosions and crusted areas seen affecting one side of face and scalp.