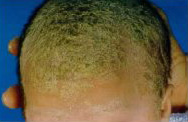
The cause of seborrhoeic dermatitis is unknown. There are two types of seborrhoeic dermatitis: (i) infantile seborrhoeic dermatitis (Fig. 1) - commonly seen in newborns and babies, (ii) adult seborrhoeic dermatitis - commonly seen in middle-aged adults.
Seborrhoeic dermatitis presents with yellowish, greasy scales on the scalp. The underlying scalp skin is red. In mild disease only patchy areas of the scalp are affected. In more severe cases, there may be diffuse scaliness and redness. Seborrhoeic dermatitis may affect the skin over the eyebrows, inner cheeks, chest, back and the groin. The condition may or may not be itchy. Seborrhoeic dermatitis is not a fungal infection although yeast infections have been reported to be associated with seborrhoeic dermatitis. Patients with HIV infection may develop very severe seborrhoeic dermatitis.
Treatment of seborrhoeic dermatitis consists of mild antiseptic or antifungal shampoos and mild topical steroid lotion or gel. The condition tends to be recurrent.