Diabetic Dermopathy
This is the commonest skin disease seen in diabetics. Skin signs are commonly found over the shins and appear as brown scars. The brown spots may be preceded by red or blistering spots. The cause is due to abnormal changes of small blood vessels in the skin. There is no specific treatment for this skin disorder. The condition tends to heal by itself into depressed scars.
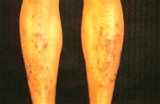
Fig. 1 Thin brown scars of diabetic dermopathy
Gangrene
Occlusion of large vessels in the feet due to diabetes can cause pain on prolonged walking as a result of poor blood circulation. Severe occlusion can lead to gangrenous changes of the toes as a result of tissue death. Surgery will be needed to remove the dead tissues and in severe cases, amputation of the foot or leg.
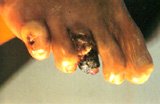
Fig. 2 Gangrenous toe as a result of tissue death
Diabetic neuropathy
Diabetes can damage the nerves resulting from occlusion of blood vessels to the nerves. This can cause a burning and tingling sensation and numbness of the feet. Patients also have reduced or loss of pain sensation and may develop skin sores and ulcers on the feet due to trauma if good foot care is not instituted.
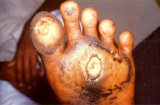
Fig. 3 Diabetic foot with neuropathic ulcer, as a result of loss of pain sensation.
Skin Infections
Diabetics are more prone to skin infections. Examples are styes, boils and fungal infection. Some infections can be serious and require immediate medical attention eg. carbuncles, which are deep bacterial infections of the hair follicle (abscess) (Fig. 4) and cellulitis which is a deep skin infection. Cellulitis often presents as a red, hot and tender swelling of the leg (Fig. 5). Necrotising fasciitis is a serious and life- threatening skin infection which may extend deep down to the muscles and requires immediate treatment and surgery. It presents as painful, inflammed haemorrhagic swelling or blistering of the skin (Fig. 6)
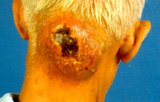
Fig. 4 Carbuncle on the neck.
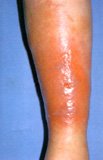
Fig. 5 Cellulitis, often resulting from entry of bacterial into the skin from trauma
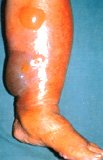
Fig. 6 Necrotising fasciitis. A serious, life- threatening infection presenting as inflammed, haemorrhagic swelling and blistering.
Necrobiosis Lipoidica
This is a rare complication of diabetes, again due to small blood vessel disease of the skin. Skin lesions usually appear on the shin. The affected skin has a reddish brown border with a yellowish centre. Sometimes, the onset of this skin disease may precede the diagnosis of diabetes and so patients with this skin disorder need to be screened for diabetes.
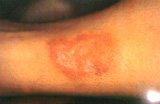
Fig. 7 Necrobiosis Lipoidica with characteristic reddish brown margin and yellowish centre
Acanthosis nigricans
This is a skin manifestation of diabetes mellitus. It is also a skin sign of other internal diseases including some hereditary diseases and internal cancer. It is commonly seen in those who are obese. Skin changes are characterised by dark, brownish black velvety thickening of the skin folds such as the armpits, upper back, neck and groins.

Fig. 8 Acathosis nigricans. Pigmented velvety thickened skin over the armpit.
Xanthomas and Xanthelasma
Diabetics often suffer from high lipid (cholesterol and triglycerides) levels in the blood. This causes fats to be deposited in the skin and presents as xanthomas or xanthelasma.
Xanthomas are symptomless yellow firm nodules usually found over bony elbows, knees and heels. Sometimes, the appearance may be as pin-head sized yellow lumps, appearing in crops over the buttocks (eruptive xanthomas) (Fig. 9). Xanthelasma is a sign of high cholesterol levels in the blood and presents as yellow patches on the eyelids (Fig. 10). Treatment is aimed at normalising the lipid levels by dietary restriction of satuarated fats and if necessary, medical treatment with lipid lowering drugs.

Fig. 9 Eruptive xanthomas, seen commonly over the buttocks. A sign of raised blood lipids.

Fig. 10 Xanthelesma on the eyelids.
Granuloma annulare
This is a skin disease seen usually in children and young adults. It is occasionally associated with diabetes. Skin signs are characterised by red spots in the initial stages which expand outwards in a ring-like fashion. The hands, especially the fingers, and elbows are commonly affected. When granuloma annulare is widespread it may be associated with underlying diabetes mellitus. The skin lesions may precede the symptoms and signs of diabetes mellitus. Patients with widespread granuloma annulare need to be screened for diabetes mellitus.
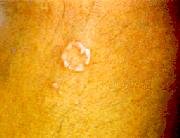
Fig. 11 Typical ring-like lesion with beaded margin of granuloma annulare.